Breastfeeding and your child’s lung malformation surgery
If you are breastfeeding your baby or child at the time they go through lung malformation surgery, a little preparation in advance can make a stressful day easier to navigate. Here is everything you need to know.
You will be separated from your child
During surgery your child will typically be in the operating room and then in recovery for anywhere from two to six hours, sometimes longer depending on the complexity of the procedure. During this time you will not be able to nurse. This means you will need to plan for how you will express milk, and how you will manage your supply and comfort during that window.
Bring your pump
In most hospitals — in the US, UK, and elsewhere — you cannot rely on the hospital to provide you with a breast pump. While some NICUs and pediatric units do have hospital-grade pumps available, this is not universal and is not something you should assume. Ask ahead and, if needed, bring your own pump and everything you need to use it: power adaptor, all pump parts, milk storage bags or bottles, and a small cooler bag with ice packs for transporting expressed milk home if needed.
If you are in the UK, some NHS trusts do have pumps available for parents of inpatient children, but provision varies significantly between hospitals. Contact your surgical team or the ward in advance to ask. Do not assume.
If you are in the US, provision varies between institutions. Again, ask in advance. Some children's hospitals, particularly those with dedicated family support programmes, will have pumps available. Others will not.
In both countries, there is no legal requirement for hospitals to provide pumping equipment to parents of inpatient children (as distinct from their own employees), so asking ahead is essential.
Finding somewhere to pump
Most hospitals will have a private space available if you ask — a family room, a quiet room, or a lactation room. In the UK, the Equality Act 2010 protects breastfeeding women from discrimination in public places including hospitals, which means a hospital cannot refuse you access to a suitable space. In the US, protections vary by state but most hospitals have family-friendly policies regardless of legal requirements. Ask the nursing staff or surgical coordinator when you arrive.
If you have never used a pump before
Surgery day is not the day to figure out how a pump works for the first time. If you have been exclusively nursing and have never expressed, we strongly recommend getting familiar with your pump in the week or two before the operation. This gives you time to:
Learn how the pump parts fit together and how to use them comfortably
Understand your own letdown and flow
Build a small supply of expressed milk in advance (see below)
Troubleshoot any issues while you are at home and not under stress
Even a few practice sessions will make a significant difference on the day.
Building a small supply in advance
Having some expressed milk already stored before surgery day means you are not under pressure to produce on an already emotionally and physically demanding day. Even a small stash (just a few feeds' worth) gives you and your baby a buffer.
How to store expressed milk safely:
At room temperature: Freshly expressed breast milk can be left at room temperature (up to 77°F / 25°C) for up to four hours. In the UK, the NHS guidance allows up to six hours at room temperature. If you are not going to use it within that window, refrigerate or freeze it promptly.
In the fridge: Breast milk can be stored in the refrigerator for up to four days. NHS guidance allows up to eight days at 4°C or lower — if you are not sure of your fridge temperature, use it within three days. Store at the back of the fridge, not in the door where temperatures fluctuate.
In the freezer: In the freezer, six months is best; up to twelve months is acceptable. Always label each bag or container with the date it was expressed. Freeze in small amounts (roughly the amount of one feed) so you can defrost only what you need without wasting any.
Thawing frozen milk: If you thaw breast milk in the refrigerator, use it within 24 hours from when it is fully thawed, not from when you took it out of the freezer. Once breast milk is brought to room temperature or warmed, use it within two hours. Never refreeze breast milk after it has thawed. Never use a microwave to heat or defrost breast milk.
In a cool bag: Breast milk that has been cooled in the fridge can be carried in a cool bag with ice packs for up to 24 hours. This is useful if you are traveling to the hospital and need to bring expressed milk with you.
On the day of surgery
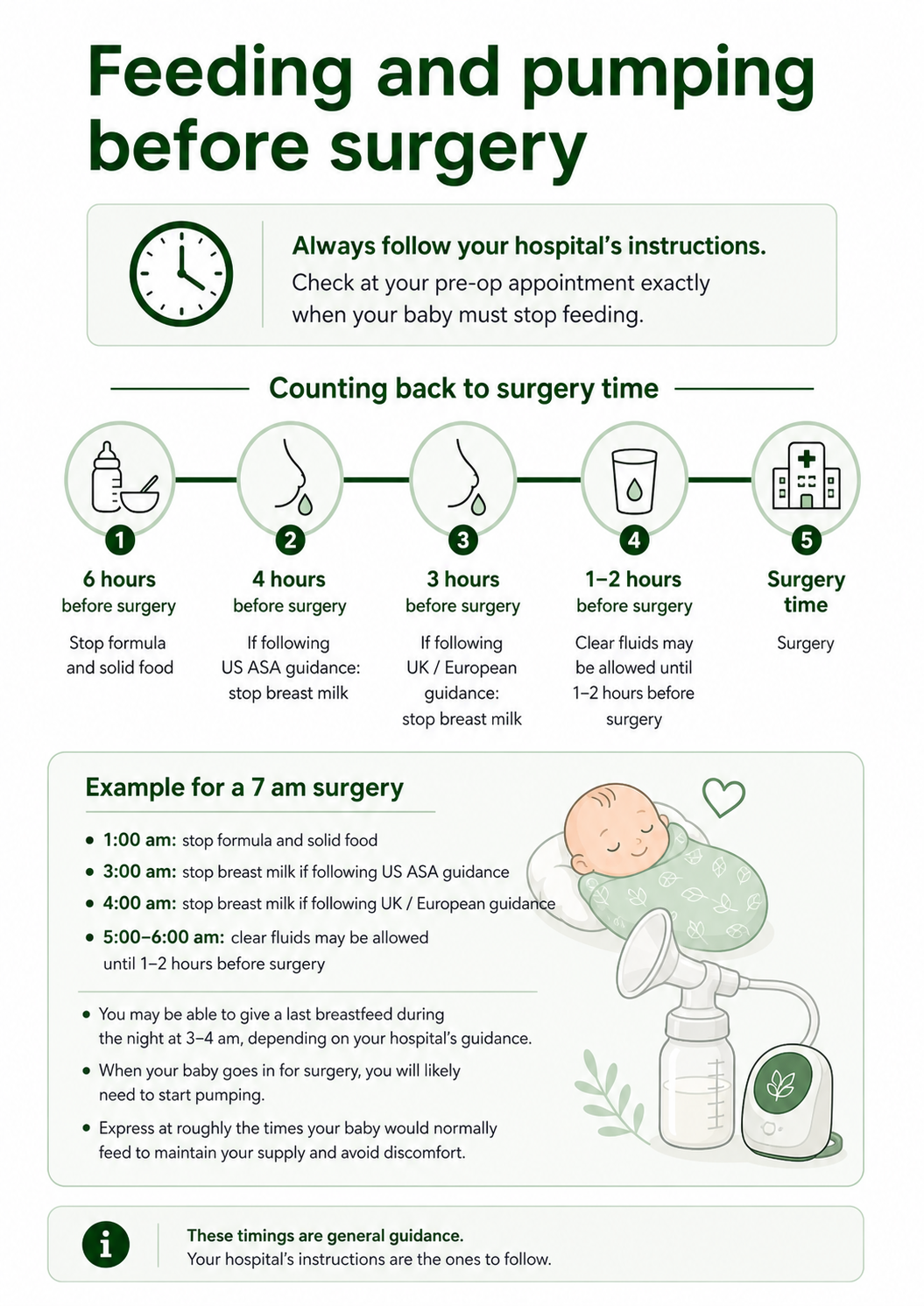
Express at roughly the intervals your baby would normally feed to maintain your supply and avoid discomfort. Your baby will need to stop eating several hours before surgery. You must check with your hospital (normally at the pre-op appointment) when they want you to stop feeding your child.
Formula and solid food normally must be stopped 6 hours before surgery
Breast milk is normally allowed until 3 hours before surgery (UK/European guidance); the US ASA guideline says 4 hours for breast milk.
Clear fluids are normally allowed until 1-2 hours before surgery
So if your child’s surgery is scheduled for 7am, you may give a last breastfeed 3-4 hours (depending on guidance) before then during the night. You will then likely need to start pumping when your child goes in for surgery.
Your surgical team can usually tell you in advance approximately how long the procedure and recovery will take, so you can plan roughly when you will need to pump.
When your child is back from recovery, your care team will let you know when you can try feeding. Some babies are able to nurse relatively soon after surgery; others will need a period of nil by mouth or will be receiving fluids in a different way initially. Your surgical and nursing team will guide you on this — if you are unsure, ask specifically when breastfeeding can resume.
A note on hospital policies
Hospital policies around pumping spaces, pump availability, and milk storage vary significantly, not just between countries but between individual hospitals. If breastfeeding is important to you and you want to be prepared, the most useful thing you can do is contact your surgical team or the ward coordinator a week or two before the operation and ask directly:
Is there a private space I can use to pump during and after surgery?
Does the ward have a pump available, or should I bring my own?
Is there a fridge I can use to store expressed milk during our stay?
Getting clear answers to these three questions in advance will remove a significant source of uncertainty on the day.
